
Hyaline Membrane Disease(HMD)
Hyaline Membrane Disease(HMD)
HMD occurs when there is not enough chemical substance called surfactant in the lungs. Surfactant is made by the cells in the airways and consists of phospholipids and protein. It begins to be produced in the fetus at about 24 to 28 weeks of pregnancy, and is found in amniotic fluid between 28 and 32 weeks. From about 35 weeks gestation, most babies have developed adequate amounts of surfactant.
- In healthy lungs, surfactant is released into the lung tissues where it helps lower surface tension in the airways, which helps keep the lung alveoli (air sacs) open.
- When there is not enough surfactant, the tiny alveoli collapse with each breath.The baby works harder and harder at breathing,trying to re-inflate the collapsed airways.
- As the baby's lung function decreases, less oxygen is taken in and more carbon dioxide builds up in the blood.This can lead to acidosis (increased acid in the blood), a condition that can affect other body organs.
- Without treatment, the baby becomes exhausted trying to breathe and eventually gives up. A mechanical ventilator (breathing machine) must do the work of breathing instead.
- The course of illness with HMD depends on the size and gestational age of the baby, the severity of the disease, the presence of infection, whether or not the baby has a patent ductus arteriosus (a heart condition) and whether or not she/he needs mechanical help to breathe.
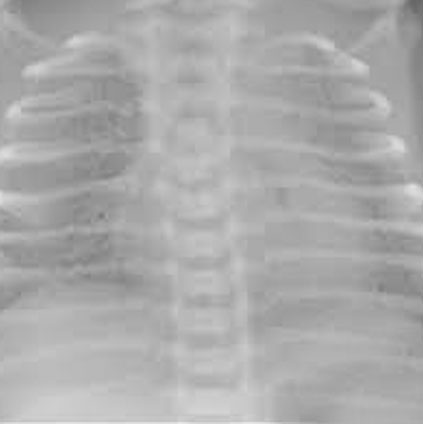
risk factors for HMD
HMD occurs in about 60 to 80 percent of babies born before 28 weeks gestation, but upto 30 percent of those born between 32 and 36 weeks also get HMD.
Although most babies with HMD are premature, other factors can influence the chances of developing the disease. These include:
- Male babies
- Previous baby with HMD
- Caesarean delivery
- Perinatal asphyxia (not breathing at birth or lack of air immediately before, during or after birth)
- Cold stress (getting cold post delivery)
- Perinatal infection
- Multiple births (Multiple birth babies are often premature)
- Infants of diabetic mothers
- Babies with patent ductus arteriosus
Symptoms of HMD
While each baby may experience symptoms differently, some of the most common symptoms of HMD include:
- Difficulty breathing at birth that gets progressively worse
- Cyanosis (blue coloring)
- Flaring of the nostrils
- Tachypnea (rapid breathing)
- Grunting sounds with breathing
- Chest retractions (pulling in at the ribs and sternum during breathing)
Symptoms of HMD usually peak by the third day. The support needed may be in the form of NICU, oxygen, CPAP or mechanical ventilation.
Complications with HMD
As with any disease, more severe cases often have greater risks for complications. Some complications associated with HMD include:
- Pneumomediastinum - air leaks into the mediastinum (the space between the two pleural sacs containing the lungs).
- Pneumothorax - air leaks into the space between the chest wall and the outer tissues of the lungs
- Pneumopericardium - air leaks into the sac surrounding the heart
- Pulmonary interstitial emphysema (PIE) - air leaks and becomes trapped between the alveoli, the tiny air sacs of the lungs
- Chronic lung disease (also called bronchopulmonary dysplasia)
- The best way of preventing HMD is by preventing a preterm birth.
- When a preterm birth cannot be prevented, giving the mother medications called corticosteroids before delivery has been shown to dramatically lower the risk and severity of HMD in the baby.
- These steroids are often given to women between 24 and 34 weeks gestation who are at risk of early delivery.
Air leaks of the lung tissues such as:
Prevention of HMD: